Capabilities of cloth masks didn’t change, why did the messaging?
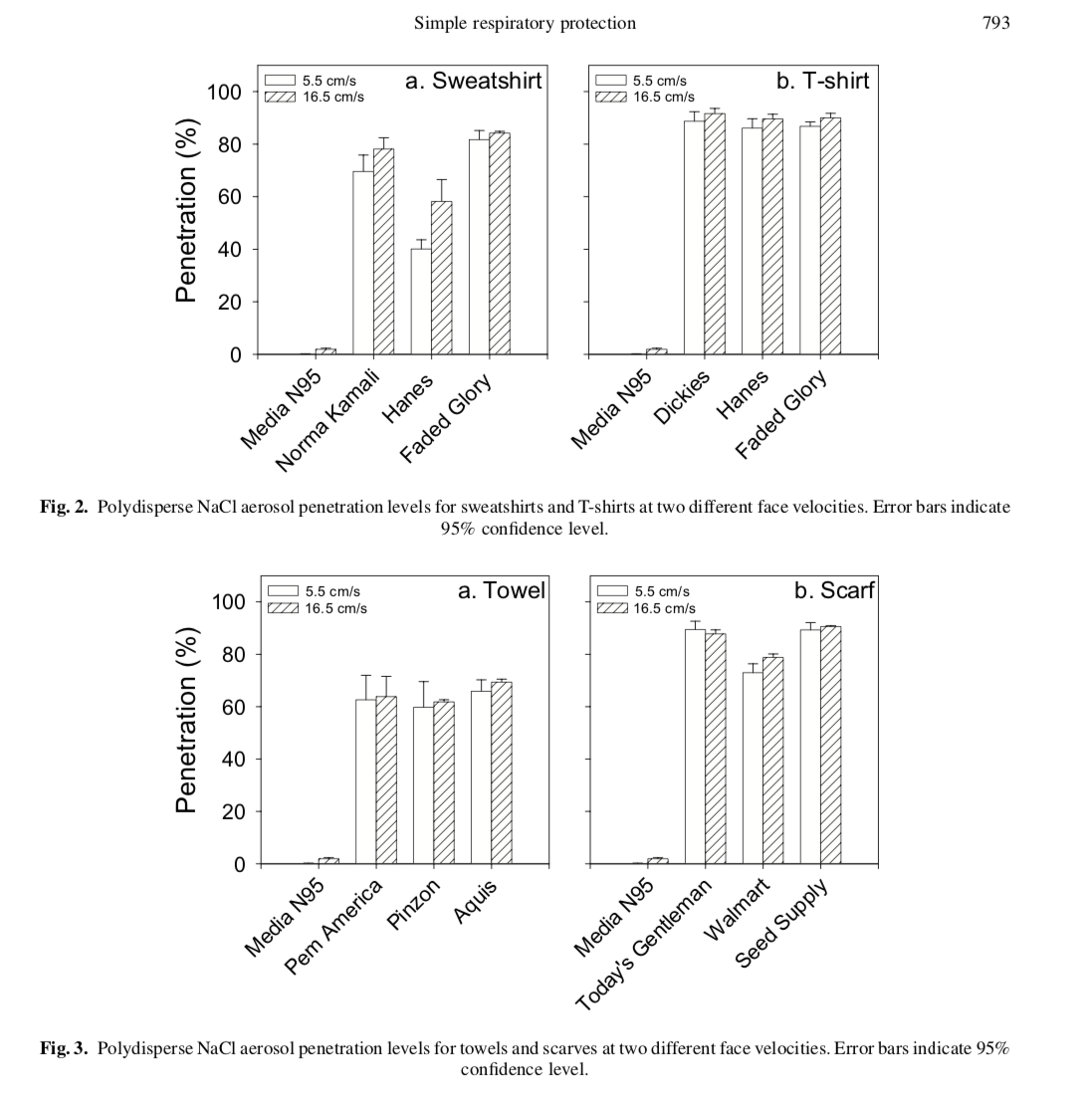
ICWA has been monitoring the face-mask issue for several months. One of the first and best papers we found regarding mask material and type was published in 2010. The study looked at “the filtration performance of common fabric materials against nano-size particles including viruses” which they compared with the penetration levels for N95 respirators (which aren’t 100% protective). They were looking at aerosol particles in the 20–1000 nm range, which would include SARS-CoV-2 (60 to 140 nm), the virus that causes COVID-19. They concluded:
“The penetration values obtained for common fabric materials indicate that only marginal respiratory protection can be expected for submicron particles taking into consideration face seal leakage.”
Add the repeated touching of the masks in real-world settings, and the evidence is against the general public wearing them to prevent the spread of any infection.
In the beginning of the COVID-19 outbreak, masks for the general public were not recommended by U.S. federal disease experts. Here is Dr. Fauci advising against use by the general public in March. In this 60 Minutes interview, Dr. Fauci agrees that masks worn by the general public collect “schmutz” which is touched and spread.
On April 1, 2020, Dr. Brosseau, a national expert on respiratory protection and infectious diseases and professor (retired), and Dr. Sietsema also an expert on respiratory protection and an assistant professor, both at the University of Illinois at Chicago, published a lengthy commentary online at CDRAP, the Center for Infectious Disease Research and Policy. They looked at the data available on Covid 19, at the historical use of masks, at many studies about mask capabilities and effectiveness in real world settings.
They concluded:
“Data lacking to recommend broad mask use
We do not recommend requiring the general public who do not have symptoms of COVID-19-like illness to routinely wear cloth or surgical masks because:
- There is no scientific evidence they are effective in reducing the risk of SARS-CoV-2 transmission
- Their use may result in those wearing the masks to relax other distancing efforts because they have a sense of protection
- We need to preserve the supply of surgical masks for at-risk healthcare workers.
Sweeping mask recommendations—as many have proposed—will not reduce SARS-CoV-2 transmission, as evidenced by the widespread practice of wearing such masks in Hubei province, China, before and during its mass COVID-19 transmission experience earlier this year. Our review of relevant studies indicates that cloth masks will be ineffective at preventing SARS-CoV-2 transmission, whether worn as source control or as PPE.”
And yet, the messaging about the general public wearing masks began to change from public health officials. The reason given was asymptomatic transmission.
While it is good to see the Surgeon General provide new guidance based on new evidence–we respect public health officials who aren’t afraid to change recommendations when new information comes along–there are a couple missing details:
- the evidence he spoke of came from computer modeling, not real-world contact tracing of asymptomatic individuals
- there was no evidence that asymptomatic transmission was happening in general public settings, such as in grocery stores or offices or sidewalks, where sustained close-up exchange of breath doesn’t happen (see end of this post for evidence it is not happening)
- cloth and surgical masks still do not effectively block viruses as small as SARS-COV-2
- cloth and surgical masks worn by the general public are still “schmutz” collectors, frequently touched, becoming sources of transmission
Since April 1, there have been several modeling studies published that conclude general mask wearing could help prevent the spread of infection, but none of these studies took any measurements in real-world settings. They were models, not real data. They did not measure “the aerosol emission upward and downward from the mask” like a 2012 study did. They did not take real-world measurements of any viruses in the moisture collected on the surfaces of the masks, on the wearer’s surrounding skin, neck, forehead, and hands, and most importantly, they did not count how many times in real-world settings masks of all types were touched, nor measure any virus transfer from the mask to the hands and to touched objects.
One of the newest modeling studies (again, no real-world measurements) that is being cited every to support universal masking, concludes that everyone in the general public should immediately begin wearing masks of any type, with the goal of getting everyone a medical standard surgical or N95 respirator as soon as possible.
We conclude that facemask use by the public, when used in combination with physical distancing or periods of lock-down, may provide an acceptable way of managing the COVID-19 pandemic and re-opening economic activity. These results are relevant to the developed as well as the developing world, where large numbers of people are resource poor, but fabrication of home-made, effective facemasks is possible. A key message from our analyses to aid the widespread adoption of facemasks would be: ‘my mask protects you, your mask protects me’.
Home-made effective facemasks? Define effective. Able to block viruses? They still can’t do that. The physics of virus blockage by materials has not changed. Able to catch a sneeze? Yes, but there are lots of ways to catch coughs and sneezes without continual mask-wearing, such as utilizing the crook of your arm, as we’ve all been taught to do. And that “key message” about wearing a mask to protect others is familiar — where have we heard it before? We heard the surgeon general say it as part of his public health messaging. And as importantly, it’s a version of the marketing messaging that has been used for vaccines for years, even for the vaccines that don’t actually prevent infection, colonization and transmission. It’s a very clever (but inaccurate) public health and drug marketing strategy. In a free country, you can’t force individuals to take an action — like wearing a mask or getting a vaccine — to protect their own health, the laws only allow for force (such as mandates) to be used when an individual’s actions may harm someone else. What better way to inspire action than to condition the public with “you do it for me, I do it for you.” These social marketing strategies don’t actually have to have scientific support to get compliance, they just have to be well-financed and distributed by major media, with some questionable “scientific” studies and articles thrown in to attempt to give them legitimacy. Add recruiting the public to be fear and shame spreaders, and you have yourself a formidable force to stand in opposition to any attempt at critical or rational dialogue.
Since the science does not support general public mask wearing, then this about-face in messaging must be part of a “Public Health Message Strategy” — meant to, what? Make people feel like they are helping? Given them a sense of security, albeit false? Keep them aware of COVID so they don’t let go of fear and start living life normally before the much-hyped and rushed and controversial billion-dollar drive to produce billions of doses of vaccines without adequate testing? Because the messaging will soon change. There will be headlines. Those highway overpass signs that now say “stay home, stay healthy” will begin to say “vaccinate to protect others” and other slogans that push for pride in being part of the “community immunity” movement. Disregarding, of course, the fact that the government has been trying very hard to prevent natural community immunity from happening.
The public is being told that the inconvenience, discomfort, ineffectiveness, even the potential for self-harm (keep reading to learn more about that) of mask-wearing at work and whenever out in public — those are things we humbly accept to protect each other? Like, there are no other common sense things people can do to stay healthy and not spread germs?
The modeling study referenced above says that for anything less than near universal adoption of quality masks worn properly (impossible to achieve in real-world situations), those who wear them incur a “susceptibility penalty.” See if you can make sense of the below paragraph from the study.
We see that if facemask wearing were to incur a susceptibility penalty—with the fomite [any inanimate object that, when contaminated with or exposed to infectious agents, can transfer disease to a new host] parameter increased by 100% and no protection against droplet inhalation, while retaining the 50% reduction in droplet exhalation—there is still a net benefit to the population. In this scenario, the mask wearers are personally worse off until about 65% of the population is wearing masks, at which point even the facemask wearers become better off than if nobody in the population was wearing facemasks (figure 8b). When compliance and facemask wearing are very bad (300% increase in fomite susceptibility with only the 50% reduction in droplet exhalation), non-mask wearers are at an advantage, but a highly counterintuitive finding is apparent in that, until about 80% facemask adoption, there is still a net benefit to the population as a whole, and a greater benefit for non-mask wearers. This non-intuitive result is due to the fact that, while an individual is made much more susceptible, this is more than counteracted by the reduced infectiousness of many individuals. These facemask wearers are more likely to contract the disease, but less likely to infect others (particularly non-facemask wearers) once infected. When most of the population is wearing these facemasks, the effect of reduced infectiousness is outweighed by the fact that the majority of the population is much more susceptible. In the unlikely eventuality of facemasks with this property, it would be advisable to preferentially issue these masks to individuals less vulnerable to severe complications, leaving more vulnerable individuals unmasked in order to maximize overall benefits, while still achieving a lower level of infection within the population.
Huh. Well then. That’s as clear as fomite schmutz smeared on a face shield.
If you’d like to explore the negative health aspects of continual face-mask wearing, here is one article that include citations to explore: Blaylock: Face Masks Pose Serious Risks To The Healthy. And we haven’t even touched on the emotional and psychological impact of mask wearing.
What is the latest evidence on asymptomatic transmission?
Maria Van Kerkhove of the World Health Organization recently reported that actual real-world contact-tracing studies of known asymptomatic carriers are finding that asymptomatic transmission is “very rare”. The media and some public health officials didn’t like the sound of that and challenged her, and then headlines saturated the media claiming she “back pedaled” the next day. But she did not take back her comment, she stood firmly by it, only adding that in the past, computer modeling estimated maybe 40% of transmission may be due to asymptomatic transmission. Computer modeling. Like the modeling that grossly overestimated the fatality risk of SARS-COV-2?
REAL WORLD tracing and testing of asymptomatic people is not showing that at all. Real world studies are showing that asymptomatic transmission is very rare, and then only in situations with close proximity for a sustained amount of time, just as households.
And then we have this in early June, 2020: AN EVIDENCE SUMMARY OF PAEDIATRIC COVID-19 LITERATURE
Precise details regarding paediatric transmission cannot be confirmed without widespread sero-surveillance, however important trends are emerging. Low case numbers in children suggest a more limited role than was initially feared. Contact tracing data from Asia, the USA, Europe and Israel have all demonstrated a significantly lower attack rate in children than adults, including testing of asymptomatic household contacts on both PCR and serology. Coupled with low case numbers would suggest that children are less likely to acquire the disease. The role of children in passing the disease to others is unknown, in particular given unknown numbers of asymptomatic cases. Notably, the China/WHO joint commission could not recall episodes during contact tracing where transmission occurred from a child to an adult. Studies of multiple family clusters have revealed children were unlikely to be the index case, in Guangzhou, China, Israel, the USA, Switzerland and internationally. Limited data on positive cases in schools have not demonstrated significant transmission. A SARS-CoV2 positive child in a cluster in the French alps did not transmit to anyone else, despite exposure to over 100 people.
So real-world evidence is showing that . . .
-
masks don’t prevent the spread of infection when used by the general public
-
asymptomatic transmission is very rare
-
children are very rarely vectors of transmission
-
99.5% of the population is not at risk of severe disease or fatality
-
and there are existing effective treatments that are saving lives (see posts HERE)
The authors of an article published in the New England Journal of Medicine on May 21, 2020, state:
“We know that wearing a mask outside health care facilities offers little, if any, protection from infection. Public health authorities define a significant exposure to Covid-19 as face-to-face contact within 6 feet with a patient with symptomatic Covid-19 that is sustained for at least a few minutes (and some say more than 10 minutes or even 30 minutes). The chance of catching Covid-19 from a passing interaction in a public space is therefore minimal. In many cases, the desire for widespread masking is a reflexive reaction to anxiety over the pandemic.”
Here is a common sense and respectful approach: How about we encourage individual choice, encourage education so that those who are at risk of severe disease don’t take chances because of a false sense of security around masked people. How about everybody with symptoms stays home and everyone without symptoms use their preferred method of blocking any random cough or sneeze, like with a tissue followed by hand washing, or the crook of their arm if hand-washing or tissue not handy.
In the above noted article by Dr. Blaylock, he states:
“It is evident from this review that there is insufficient evidence that wearing a mask of any kind can have a significant impact in preventing the spread of this virus. The fact that this virus is a relatively benign infection for the vast majority of the population and that most of the at-risk group also survive, from an infectious disease and epidemiological standpoint, by letting the virus spread through the healthier population we will reach a herd immunity level rather quickly that will end this pandemic quickly and prevent a return next winter. During this time, we need to protect the at-risk population by avoiding close contact, boosting their immunity with compounds that boost cellular immunity and in general, care for them.
One should not attack and insult those who have chosen not to wear a mask, as these studies suggest that is the wise choice to make.”
We agree 100%.
And let’s not forget the most important thing — we are symbiotic creatures. We are more viral than we are human. We have immune systems that protect us, with layers and stages of protection. Healthy people with healthy hygiene habits contribute to a healthy society and are able to slow or block the transmission of infection because they themselves are NATURALLY resistant. To read about the nutrients and therapies experts are recommending to increase your own natural health and infection resistance, search our posts on our COVID-19 page.

